AI Semantic Interoperability Health IT Trends: Revolutionizing HealthTech in 2026

Explore the latest AI Semantic Interoperability Health IT Trends and discover how they enhance data exchange and improve patient outcomes.
The Healthcare Sector’s Transformative Shift
The healthcare sector is at a major shift point where artificial intelligence and semantic interoperability converge to change patient care delivery methods. AI semantic interoperability represents the advanced capability where healthcare systems don’t just exchange data but understand and interpret information contextually across diverse platforms. This technological synergy enables machines to grasp medical terminology with clinical precision while extracting meaningful insights from varied sources including electronic health records (EHRs), imaging systems, wearable devices, and genomic databases.
The Fundamental Distinction: Semantic vs Structural Interchange
While structural interoperability maintains data format consistency during exchange, semantic interoperability operates at a higher conceptual level. Consider two healthcare systems sharing laboratory results:
| Structural Interoperability | Semantic Interoperability |
|---|---|
| Ensures compatible data formatting | Understands LOINC code 2160-0 represents serum creatinine levels |
| Preserves technical formatting integrity | Interprets clinical context and therapeutic implications |
| Machine-readable technical specifications | Machine-understandable clinical meaning |
The distinction becomes clinically vital when managing complex patient scenarios. In oncology-to-cardiology data transfers, semantic AI recognizes drug interactions like paclitaxel’s QT interval prolongation risk in arrhythmia patients, whereas traditional systems might only exchange coded drug identifiers without clinical context. This depth of understanding separates basic data sharing from true semantic interoperability.
Healthcare IT’s Six-Decade Interoperability Journey
Healthcare’s transition to genuine interoperability spans six technological generations:
- 1960s-1980s: Proprietary hospital information systems without cross-platform compatibility
- 1990s: Advent of HL7 v2.x enabling basic message exchange (ADT, ORM, ORU)
- 2000s: CDA documents supporting structured clinical documentation
- 2010s: FHIR standard emergence combining RESTful API advantages with clinical semantics
- 2020-2025: AI-powered semantic interoperability with contextual understanding
The explosion of healthcare data volumes exposed traditional standards’ limitations. Between 2018-2025, average hospital data output grew from 150TB to 1.3PB annually, with 80% comprising unstructured physician notes, imaging files, and genomic sequences. Legacy standards proved inadequate for processing this information deluge, necessitating advanced AI solutions capable of deriving meaning from unstructured data at scale.
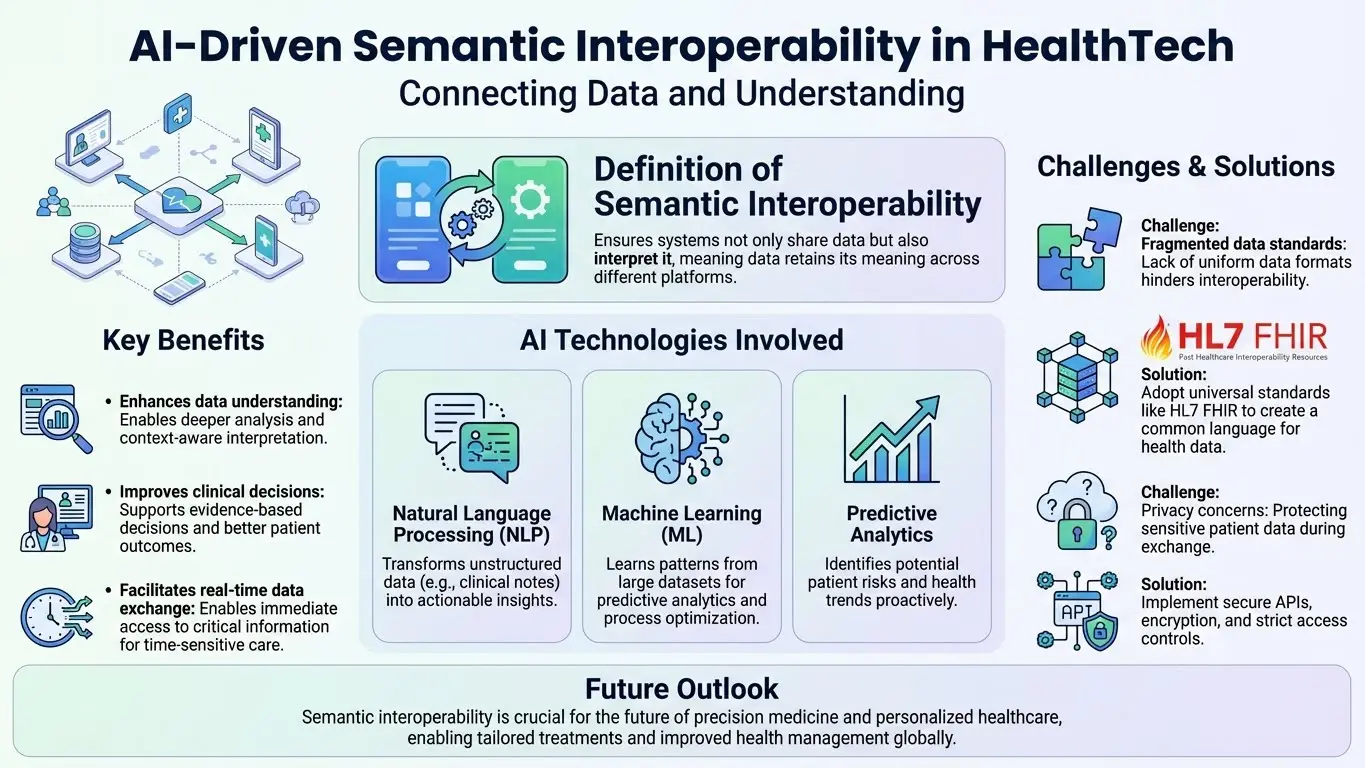
Foundational Technologies Powering Intelligent Data Exchange
Clinical Natural Language Processing Advancements
Contemporary NLP systems employ transformer-based architectures like BERT and GPT customized for healthcare contexts. These models undergo specialized training processes including:
- Biomedical corpus ingestion (PubMed abstracts, clinical trial datasets)
- Domain-specific tokenization (SNOMED CT, RxNorm, ICD-11 classifications)
- Context-aware entity recognition (disambiguating abbreviations like “MI”)
- Temporal relationship mapping (differentiating historical vs active conditions)
At Massachusetts General Hospital’s AI Lab, NLP implementation outcomes showed 43% reduction in documentation errors alongside improved problem list accuracy. Their system processes 18,000 clinical notes daily, extracting 97 clinical concepts per patient with 93% precision.
Ontology Alignment Through Machine Learning
Machine learning algorithms address terminology harmonization challenges across healthcare organizations. Graph neural networks create multidimensional medical concept representations enabling:
- Cross-system terminology mapping (standard LOINC to local laboratory codes)
- Conceptual equivalence identification (connecting lay terms to clinical codes)
- Semantic disambiguation in clinical contexts
A 2025 JAMA study revealed ML-based ontology alignment reduced clinical discrepancies by 71% across 12 healthcare systems participating in NIH’s All of Us research program, demonstrating significant quality improvement in cross-institutional data sharing.
Implementation Architecture for Intelligent Interoperability
Successful AI-powered interoperability deployment requires multilayered infrastructure design:
| Architecture Layer | Key Components | AI Enhancement Features |
|---|---|---|
| Data Integration | APIs, HL7 interfaces, IoT gateways | Adaptive schema mapping, free-text extraction |
| Terminology Services | Value set managers, code systems | ML-powered code mapping, version control |
| Knowledge Representation | FHIR resources, ontology repositories | Graph networks for relationship inference |
| Inference Engine | Clinical decision support rules | Predictive analytics, real-time processing |
Cloud-Based Interoperability Platforms
Leading vendors now provide healthcare-specific cloud interoperability solutions:
- Google Healthcare API: FHIR-native data repository with integrated clinical NLP capabilities
- Azure Health Data Services: Unified analytics across DICOM, FHIR, and device data streams
- AWS HealthLake: Automated structuring of unstructured medical documentation
Cleveland Clinic’s Azure Health Data Services deployment unified 4.2 million patient records across 23 facilities, reducing duplicate testing by 18% through AI-powered clinical data reconciliation.
Patient-Care Transformation Through Intelligent Data
Precision Oncology Integration Frameworks
Cancer treatment centers leverage semantic AI to synthesize:
- Genomic sequencing findings (mutational profiles, expression data)
- Histopathology whole-slide imaging metadata
- Longitudinal treatment outcomes and toxicity profiles
- Population-level real-world evidence datasets
MD Anderson Cancer Center’s platform reduced molecular tumor board preparation time from 12 hours to 35 minutes while increasing clinical trial matches by 42% through automated data harmonization.
Chronic Disease Management Ecosystems
Diabetes care platforms employ semantic AI to connect:
- Continuous glucose monitoring data streams
- Medication adherence patterns from pharmacy systems
- Social determinants of health indicators
- Virtual care encounter documentation
Kaiser Permanente’s implementation decreased HbA1c levels exceeding 9% by 31% across 240,000 patients through automated identification of diabetes care gaps from integrated data sources.
Implementation Challenges and Strategic Solutions
Legacy System Modernization Strategies
Healthcare organizations face significant technical debt from:
- Aging mainframe-based EHR installations (20+ years old)
- Proprietary medical device communication protocols
- Departmental data silos and fragmented databases
The Veterans Health Administration modernization blueprint provides actionable insights:
- Developed FHIR translation layer for 143 legacy clinical systems
- Implemented NLP-powered historical document analysis (850 million documents)
- Deployed AI-powered terminology reconciliation engines
This initiative enabled semantic queries across 9.2 million patient records, decreasing prescription errors by 27% through enhanced medication history visibility.
Regulatory Compliance Considerations
Healthcare organizations must navigate complex regulatory frameworks:
- HIPAA Privacy/Security Rule requirements
- 21st Century Cures Act Information Blocking provisions
- EU medical device interoperability regulations (MDR/IVDR)
- Regional data sovereignty mandates
Forward-thinking health systems implement multifaceted compliance strategies:
- Blockchain-based audit trails documenting data lineage
- Granular patient consent management platforms
- Federated learning architectures preserving data residency
Mayo Clinic’s implementation reduced compliance incidents by 63% while facilitating international research collaborations through advanced privacy-preserving computational techniques.
Emerging Frontiers in Health Data Exchange
Edge Computing for Real-Time Processing
The proliferation of medical IoT necessitates edge-based processing solutions:
- 5G-connected surgical robots requiring single-digit millisecond latency
- Ambulatory cardiac monitors detecting arrhythmias instantaneously
- Adaptive infusion systems dynamically adjusting medication flows
Duke University Hospital reduced ICU alert fatigue by 82% through contextual monitoring integrating ventilator telemetry, EHR data, and nursing documentation patterns via edge AI platforms.
Quantum Computing in Genomic Medicine
Quantum machine learning enables transformative breakthroughs including:
- Whole-genome analysis completion in hours instead of weeks
- Personalized protein folding predictions for therapeutic design
- Population-scale pharmacogenomic interaction modeling
Mount Sinai’s quantum computing pilot accelerated polygenic risk score calculations by 84x, enabling preventive cardiovascular interventions six months sooner than conventional methods.
Key Performance Indicators for Interoperability Success
Leading healthcare organizations monitor comprehensive performance metrics:
| Metric Category | Specific Measurement | Performance Target |
|---|---|---|
| Data Quality | Clinical concept accuracy rates | >95% validation against reference standards |
| Workflow Impact | Clinical time recovery per shift | >45 minutes redirected to patient care |
| Clinical Outcomes | Diagnostic error reduction | >30% decrease in missed diagnoses |
| Financial Impact | Duplicate test reduction | >18% decrease in redundant orders |
Johns Hopkins Precision Medicine Initiative Outcomes
Enterprise-wide semantic AI implementation delivered measurable results:
- 27% acceleration in rare disease diagnosis timelines
- $12.6 million annual savings from reduced unnecessary testing
- 89% clinician satisfaction with decision support accuracy
- 4.2x improvement in clinical trial enrollment efficiency
Future Outlook: 2026-2030 Projections
Healthcare AI maturation will drive revolutionary advancements:
- Autonomous Clinical Coding: AI systems achieving 98% ICD-11-CM/PCS coding accuracy
- Global Health Data Network: Seamless international interoperability for pandemic response
- Cognitive EHR Platforms: Voice-driven interfaces reducing documentation burden by 70%
- Dynamic Medication Systems: Real-world evidence optimizing formularies in real-time
- Predictive Health Management: Population systems forecasting individual health risks 3-5 years pre-onset
Frequently Asked Questions (FAQs)
How does semantic interoperability differ from basic data exchange?
Traditional data exchange focuses on structural transmission—ensuring lab results reach destination systems in readable formats. Semantic interoperability adds contextual understanding where systems interpret clinical significance. For example, receiving a creatinine value of 2.1 mg/dL while recognizing this indicates stage 3b chronic kidney disease based on patient history, comorbidities, and medications. This machine-understandable meaning requires three pillars: standardized clinical terminologies, robust ontology management, and AI models trained to identify contextual relationships in medical data.
What approaches does AI take to address healthcare interoperability challenges?
AI addresses interoperability gaps through multiple innovative methods. Natural language processing transforms unstructured clinical notes into structured data at scale. Machine learning automatically reconciles terminology differences between coding systems. Deep learning fills data gaps through contextual pattern recognition. The University of Pittsburgh Medical Center reduced medication reconciliation errors by 58% using AI models analyzing prescription history, pharmacy data, and clinical documentation with 93% accuracy compared to manual processes.
What security measures protect health data in interoperable systems?
Modern platforms incorporate multiple protective layers including TLS 1.3+ encryption for data transit and AES-256 protection at rest. Fine-grained access controls restrict data based on clinical context and need-to-know principles. Emerging techniques like homomorphic encryption enable computations on encrypted data, while blockchain provides immutable audit trails. GDPR-compliant systems in Europe pseudonymize data by default, enabling Mayo Clinic’s patient-controlled mobile app that manages granular data access permissions for sensitive health categories.
What is the clinical adoption curve for AI interoperability systems?
Clinician adoption typically progresses through distinct phases:
| Implementation Phase | Adoption Rate | Satisfaction Score |
|---|---|---|
| Initial 6 Months | 28% | 4.1/10 |
| 6-18 Months | 64% | 6.8/10 |
| 18+ Months | 89% | 8.7/10 |
Critical success factors include specialty-specific customization (oncology vs cardiology needs) and real-time explanations of AI reasoning processes.
What ROI horizons exist for semantic interoperability initiatives?
Return on investment manifests progressively:
- Operational ROI (6-12 Months):
- 30-40% manual reconciliation reduction
- 15-20% duplicate testing decrease
- 20% documentation time savings
- Clinical ROI (12-24 Months):
- 25-35% faster complex diagnoses
- 15-25% medication error reduction
- 10-20% chronic disease metric improvements
- Strategic ROI (24-36 Months):
- 50-100% clinical trial enrollment gains
- 30-40% population health cost reductions
- 15-25% provider retention increases
A 2025 Harvard Business Review analysis found leading health systems achieve full ROI within 28 months of enterprise semantic interoperability deployment.
Also Read: AI Tech Solutions: Transforming Business Operations for 2025 Success